CYSVIEW®.
CONFIDENCE AT FIRST SIGHT.
Cysview (hexaminolevulinate HCL) is an innovative technology in the diagnosis non-muscle invasive papillary bladder cancer (NMIBC).
Cysview> is used with Blue Light Cystoscopy (BLC®) as an adjunct to White Light Cystoscopy (WLC) and not separately, in the detection of NMIBC in patients with known or suspected bladder cancer. Cysview can improve the detection of NMIBC beyond that achieved with WLC alone, resulting in a more complete transurethral resection of bladder tumour (TURBT). 1,2
Cysview should be considered both in the initial evaluation of suspected NMIBC and the follow-up TURBTs.2 Cysview is approved around the world (branded in the EU as Hexvix® and the US and Canada as Cysview). It is recommended by the Canadian Urology Association3, AUA/SUO Guideline on NMIBC4, and a number of expert panels.2,5,6
Read more
THE BENEFIT OF BLC WITH CYSVIEW®
Cysview has demonstrated clear benefits over WLC alone in terms of impact on clinical practice and patients’ experiences from diagnosis to cancer management.
Cysview improves the detection of papillary tumors, leading to improved detection of NMIBC that may result in better management of non-muscle invasive bladder cancer.2
Read more
THE PROCEDURE
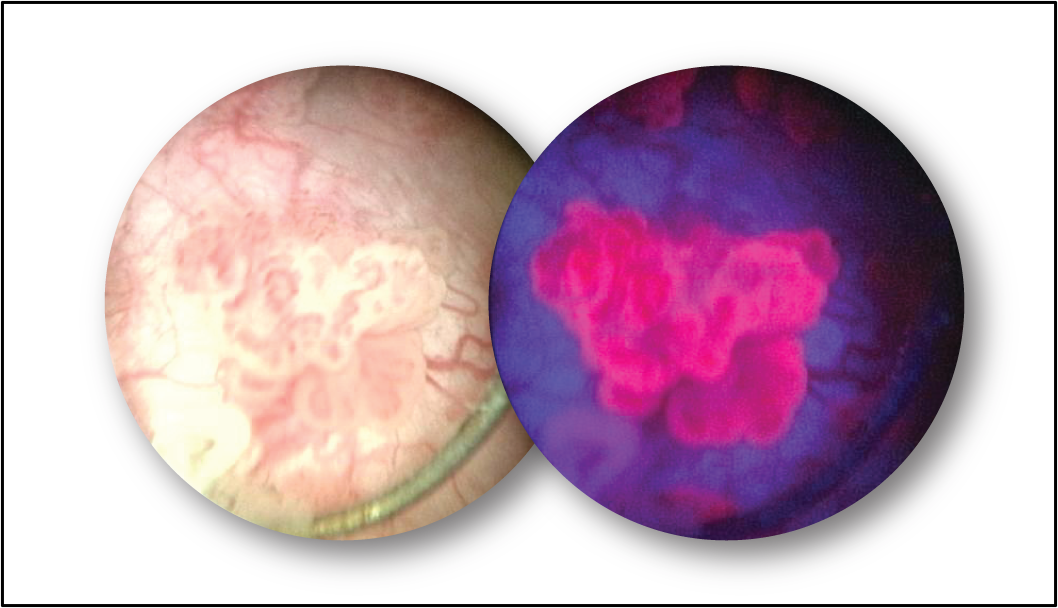
Cysview is an optical imaging agent that makes cancer cells fluoresce red/pink under blue light illumination. BLC can be performed using only approved cystoscopic machines equipped with the necessary filters to allow examination using both white light and blue light. The blue light (wavelength 360–450nm) can easily be switched on and off by the click of a button, giving doctors the benefit of both modes.
Read moreCLINICAL EVIDENCE
BLC with Cysview significantly improves the detection of papillary bladder tumours compared to WLC alone.7
The study conclusions were that BLC with Cysview "significantly improves the detection of bladder cancer leading to a more complete resection."8
Read moreIndication for Cysview® (hexaminolevulinate HCl)
Cysview is indicated as an adjunct to White Light Cystoscopy in the detection of non-muscle invasive papillary bladder cancer in patients with known or suspected bladder cancer.
Only approved cystoscopic equipment should be used, equipped with necessary filters to allow both White Light Cystoscopy (WLC) and Blue Light (wavelength 360–450nm) fluorescence Cystoscopy (BLC®). Training in Blue Light Cystoscopy with an approved Photodynamic Diagnosis (PDD) System is essential prior to the use of Cysview.
Limitations of Use Cysview is not a replacement for random bladder biopsies or other procedures used in the detection of bladder cancer.
Contraindications Cysview is contraindicated in patients with porphyria and/or hypersensitivity to the active substance or to any ingredient in the formulation or component of the container. False-positive fluorescence may result from tangential light, scope trauma from a previous cystoscopic examination, and/or bladder inflammation particularly from intravesical Bacillus Calmette–Guérin (BCG) or chemotherapy treatments. No specific drug interaction studies have been performed.
Warnings and Precautions Do not use in patients with gross hematuria. Do not use in patients at high risk of bladder inflammation, e.g., less than 90 days after intravesical BCG or chemotherapy. Do not use for retrograde uretero-renoscopy. Cysview has not been studied in pregnant women or pediatric populations. Cysview may not detect all malignant lesions. Very rare instances of hypersensitivity, including anaphylactic shock, have been reported during post-marketing use of Cysview. Advance life support facilities should be readily available. Biopsy/resect bladder mucosal lesions only following completion of both White Light and Blue Light Cystoscopy.
Adverse Reactions Most of the reported adverse reactions in clinical studies were transient and mild or moderate in intensity: bladder spasm 2.4%; dysuria 1.8%; bladder pain 1.7%; and hematuria 1.7%. The adverse reactions observed were expected based on previous experience with standard cystoscopy and TURBT procedures.
For additional information about Cysview, please refer to the product monograph.
Note: Cysview (hexaminolevulinate (HAL) HCl) is used with Blue Light Cystoscopy (BLC) as an adjunct to White Light Cystoscopy (WLC) and not separately. Cysview with BLC may be referred to in a number of ways, such as Cysview, Cysview with BLC, Cysview with Photodynamic Diagnosis (PDD) System, HAL with BLC and HAL with PDD.
- Hermann GG, Mogensen K, Carlsson S, et al. Fluorescence-Guided Transurethral Resection of Bladder Tumours Reduces Bladder Tumour Recurrence Due to Less Residual Tumour Tissue in Ta/T1 Patients: A Randomized Two-Centre Study. BJU Int. 2011;108(8b):E297-E303.
- Daneshmand S, Schuckman AK, Bochner BH, et al. Hexaminolevulinate Blue-Light Cystoscopy in Non-Muscle Invasive Bladder Cancer: Review of the Clinical Evidence and Consensus Statement on Appropriate Use in the USA. Nat Rev Urol. 2014;11(10):589-596.
- Bhindi B, Kool R, Kulkarni GS, et al. Canadian Urological Association Guideline on the Management of Non-Muscle-Invasive Bladder Cancer – Full-Text. Can Urol Assoc J 2021;15(8):E424-457.
- Chang SS,Boorjian SA, Chou R, et al. Diagnosis and Treatment of Non-Muscle Invasive Bladder Cancer: AUA/SUO Guideline. J Urol. 2016;196(4):1021-1029.
- Lotan Y, Bivalacqua TJ, Downs T, et al. Blue Light Flexible Cystoscopy with Hexaminolevulinate in Non-Muscle Invasive Bladder Cancer: Review of the Clinical Evidence and Consensus Statement on Optimal Use in the USA—Update 2018. Nat Rev Urol. 2019;16(6):377-386.
- Witjes JA, Redorta JP, Jacqmin D, et al. Hexaminolevulinate-Guided Fluorescence Cystoscopy in the Diagnosis and Follow-Up of Patients with Non-Muscle Invasive Bladder Cancer: Review of the Evidence and Recommendations. Eur Urol. 2010;57(4):607-614.
- Cysview® Canada Product Monograph, Jan 11, 2022.
- Stenzl A, Burger M, Fradet Y, et al. Hexaminolevulinate Guided Fluorescence Cystoscopy reduces Recurrence in Patients with Nonmuscle Invasive Bladder Cancer. J Urol. 2010;184(5):1907-1913.

 contact
contact